 Somewhere in a bathroom drawer or medicine cabinet, we all have one—that little plastic dental floss dispenser. And whether you use your floss every day (yay!), or have completely forgotten
Read more
Somewhere in a bathroom drawer or medicine cabinet, we all have one—that little plastic dental floss dispenser. And whether you use your floss every day (yay!), or have completely forgotten
Read more

My Blog
-
Flossing Fact or Flossing Fiction?
posted: Apr. 23, 2024.
 Somewhere in a bathroom drawer or medicine cabinet, we all have one—that little plastic dental floss dispenser. And whether you use your floss every day (yay!), or have completely forgotten
Read more
Somewhere in a bathroom drawer or medicine cabinet, we all have one—that little plastic dental floss dispenser. And whether you use your floss every day (yay!), or have completely forgotten
Read more
-
Earth Day
posted: Apr. 16, 2024.
 The idea for Earth Day was the brainchild of Gaylord Nelson, a senator from Wisconsin. He envisioned an Earth Day that would be a kind of environmental teach-in. The first
Read more
The idea for Earth Day was the brainchild of Gaylord Nelson, a senator from Wisconsin. He envisioned an Earth Day that would be a kind of environmental teach-in. The first
Read more
-
Energy Drinks and Dental Health
posted: Apr. 09, 2024.
 Are energy drinks bad for your teeth? Many of our patients at Raymond Clark DDS ask us this question, so here’s the scoop.
Energy drinks have been on the rise, taking
Read more
Are energy drinks bad for your teeth? Many of our patients at Raymond Clark DDS ask us this question, so here’s the scoop.
Energy drinks have been on the rise, taking
Read more
-
Snowball Effect
posted: Apr. 02, 2024.
 Winter and its snowball fights are behind us, true, but there might be another kind of snowball heading your way—the snowball effect you risk when small dental concerns are ignored
Read more
Winter and its snowball fights are behind us, true, but there might be another kind of snowball heading your way—the snowball effect you risk when small dental concerns are ignored
Read more
-
Anatomy of a Smile Makeover
posted: Mar. 26, 2024.
 A smile makeover is usually a combination of one or more cosmetic dental procedures. To achieve your desired result, the doctor may perform or suggest a variety of options. The
Read more
A smile makeover is usually a combination of one or more cosmetic dental procedures. To achieve your desired result, the doctor may perform or suggest a variety of options. The
Read more
-
The Purpose of a Dental Crown
posted: Mar. 19, 2024.
 A dental crown, otherwise known as a cap, covers an infected tooth and can vary in function, depending on the position of the tooth. Crowns cover all the visible parts
Read more
A dental crown, otherwise known as a cap, covers an infected tooth and can vary in function, depending on the position of the tooth. Crowns cover all the visible parts
Read more
-
St. Patrick's Day
posted: Mar. 12, 2024.
 On March 17, everyone has a little Irish in them. St. Patrick’s Day is a joyous celebration of Irish heritage. The holiday originated as a commemoration of Saint Patrick, who
Read more
On March 17, everyone has a little Irish in them. St. Patrick’s Day is a joyous celebration of Irish heritage. The holiday originated as a commemoration of Saint Patrick, who
Read more
-
Good Nutrition Leads to Healthy Mouths
posted: Mar. 05, 2024.
 At Raymond Clark DDS, we know the most common oral health diseases are tooth decay and periodontal disease (or gum disease), and both are among the easiest to prevent. One
Read more
At Raymond Clark DDS, we know the most common oral health diseases are tooth decay and periodontal disease (or gum disease), and both are among the easiest to prevent. One
Read more
-
Hypersensitive Teeth
posted: Feb. 27, 2024.
 It is common to experience dentine hypersensitivity, with symptoms ranging from moderate to severe. Why does it happen and how do you know if this sensitivity is something to be
Read more
It is common to experience dentine hypersensitivity, with symptoms ranging from moderate to severe. Why does it happen and how do you know if this sensitivity is something to be
Read more
-
What Are Chalky Teeth?
posted: Feb. 20, 2024.
 You’ve always taken care of your child’s smile. You make sure thorough brushing and flossing take place twice a day. You serve foods high in vitamins and minerals and low
Read more
You’ve always taken care of your child’s smile. You make sure thorough brushing and flossing take place twice a day. You serve foods high in vitamins and minerals and low
Read more
-
Valentine's Day History
posted: Feb. 13, 2024.
 Valentine’s Day is best known as a celebration of love in all its forms. Pink hearts, red roses, and cute greeting cards adorn every surface you see. What many people
Read more
Valentine’s Day is best known as a celebration of love in all its forms. Pink hearts, red roses, and cute greeting cards adorn every surface you see. What many people
Read more
-
In the Pink
posted: Feb. 06, 2024.
 Our gums cover and protect the sensitive roots of our teeth and the bone around them. While we often think of gum tissue as a rosy shade of pink, that’s
Read more
Our gums cover and protect the sensitive roots of our teeth and the bone around them. While we often think of gum tissue as a rosy shade of pink, that’s
Read more
-
What did the first dentures look like?
posted: Jan. 30, 2024.
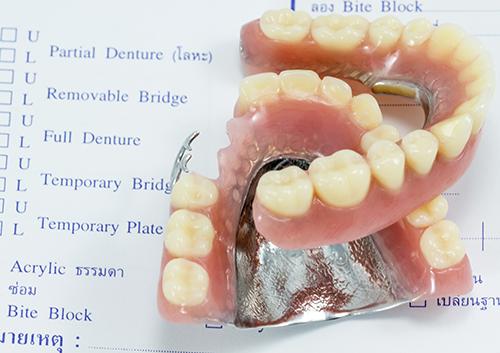 Remember hearing about George Washington and his wooden choppers? Not his tools for cutting down cherry trees, but his false teeth.
Actually, George’s teeth were made of ivory but were so
Read more
Remember hearing about George Washington and his wooden choppers? Not his tools for cutting down cherry trees, but his false teeth.
Actually, George’s teeth were made of ivory but were so
Read more
-
The Secret to Fresh Breath
posted: Jan. 23, 2024.
 Bad breath: We’ve all dealt with it. You’ve been around people who have it and, like it or not, you have had it yourself. It can be embarrassing and uncomfortable,
Read more
Bad breath: We’ve all dealt with it. You’ve been around people who have it and, like it or not, you have had it yourself. It can be embarrassing and uncomfortable,
Read more
-
Should You Get Dental Veneers?
posted: Jan. 16, 2024.
 Dental veneers are a popular treatment to improve the appearance of your smile. the doctor and our team want to help you understand whether this dental option is right for
Read more
Dental veneers are a popular treatment to improve the appearance of your smile. the doctor and our team want to help you understand whether this dental option is right for
Read more
-
How to Handle an Unexpected Dental Emergency
posted: Jan. 09, 2024.
 Regardless of the type of dental emergency you experience, it is important that you visit Raymond Clark DDS for emergency dental care as soon as possible. A chipped or cracked
Read more
Regardless of the type of dental emergency you experience, it is important that you visit Raymond Clark DDS for emergency dental care as soon as possible. A chipped or cracked
Read more